Stents (wire props) are placed within narrowed (stenotic) or blocked (blood clotted) coronary arteries that feed the heart with oxygenated blood over 2 million times a year in the U.S., mostly among men and women with angina chest pain.
The use of a coronary artery stent may sometimes be worse than the patient’s disease. The history of coronary artery stenting is one of presumed effectiveness. Stent-induced heart attacks and deaths have plagued this widely practiced intervention since its inception.
Since 1986 when the first stent (a cylindrical metallic wire device to prop open narrowing arteries that supply the heart to oxygenated blood) was implanted, it was presumed these implants were obviously effective. The Food & Drug Administration didn’t officially approve of these devices till 1994.
Given that stents do not address the cause of coronary artery disease, it is not surprising to learn of their many drawbacks.
The need for stents became apparent after balloon angioplasty that involves the insertion of a wire with a balloon tip into coronary arteries. The balloon is inflated to break up a clot in a narrowed artery. Following balloon angioplasty, rebound occlusion occurred in 5-10% of patients within minutes to hours immediately following the procedure.
Today many stents are placed in coronary arteries solely based upon symptoms of sometimes incapacitating chest pain (angina).
Stents do not completely eliminate re-stenosis, that is, recurrence of arterial narrowing, and in-stent closure or collapse is reported. In fact, within-stent narrowing (re-stenosis) is as high as 20-30% of treated cases of angina.
Drug-eluting stents then were developed to overcome that problem but long-term follow-up revealed cases of stent thrombosis (stent-induced blood clots) which is now known to induce a severe heart attack in 50% of stents that do form thrombi with an accompanying 20% mortality rate. So anti-blood clotting therapies (aspirin, heparin, warfarin) were then employed with stenting, but this led to high rates of bleeding episodes that require long hospital stays.
The use of stents has grown to the point of absurdity. One patient had 67 stents placed in his heart. The patient’s angina persisted and his cardiologist just kept implanting stents in an effort to relieve the unremitting pain. Where does this insanity stop?
All is not so happy in the land of coronary artery stents.
By 2007 the COURAGE trial shocked the cardiology profession. Stenting was no better than optimal drug therapy (aspirin, statins, blood thinners). Stenting did not reduce the rate of heart attack or death compared to medicines alone. This finding persisted through 15 years of follow-up. But the use of stents continued to rise exponentially.
More recently the stenting industry took another arrow straight through its own heart – the now infamous ORBITA trial, published in the journal LANCET in 2018.
The ORBITA trial attempted to assess the placebo effect by putting patients with angina chest pain through a mock procedure (sham surgery) with anesthesia, but no stent was implanted. Then evaluators compared them with patients who had a stent placed in a narrowed coronary artery. Neither the evaluators nor the patients knew which subjects received a stent (called a double-blind study). These patients had severe (~84%) narrowing of a coronary artery.
The angina chest pain patients who underwent stenting only gained a few seconds of pain-free time walking on a treadmill over the patients who didn’t receive a stent, which was considered insignificant. In the ORBITA trial the time it took for chest pain to occur during treadmill exercise improved from 11.8 seconds for sham surgery to 28.4 seconds with placement of a stent in a coronary artery, a statistical but meaningless improvement. Researchers had hoped for 90-120 second improvement.
This failure received widespread negative publicity. Stenting actually improved blood flow as a measure of coronary artery blood circulation (peak wall motion score) improved. So stenting was technically successful but of useless utility.
Back in the aftermath of the negative COURAGE trial, cited above, the narrative in defense of stents was repeatedly uttered by cardiologists. It sounded something like this:
“We’ve known for decades that stents don’t reduce the risk for death or heart attack in stable coronary artery disease, but that’s not why we place stents in these patients—we do it to improve symptoms and quality of life, and stenting is better than optimal medicine therapy for angina relief. Plus, many patients don’t like to take medications (or don’t want to wait for medications to work), so stents are a more effective treatment for angina, and that’s what we can offer to our patients.”
The world of denial
But after publication of the ORBITA Trial, cardiologists were left to defend their incomes with specious arguments, like the trial “wasn’t sufficiently powered” (not enough patients tested).
As Milton Packer MD states: “The results of the (ORBITA) trial threatened the livelihoods of thousands of interventional cardiologists… they criticized the trial with a vengeance,” they have placed the ORBITA trial “into the dustbin of history.”
A well-known politician once said: “’Everyone is entitled to his own opinion, but not to his own facts.” Cardiologists have created a false reality of their own. Their fallacious proposition is based upon a medical “false prop” inserted a couple million times a year into unsuspecting angina patients.
The sour story is that stent-happy cardiologists talked 85% of those naïve and fearful patients who underwent a sham operation into having a stent placed. Cardiologists use this as evidence for the popularity and preference for stents (or is this just salesmanship where doctors play on the fears of their patients?)
Another study conducted in China shows that physicians tend to subjectively over-estimate the severity of narrowed of arteries. “Born to stent” is the cardiologists’ mantra these days.
Wrong paradigm
A noted Cleveland Clinic physician says the “clogged pipe” analogy used to describe disease in coronary arteries and justify the need for stents is flawed. Dr. Michael B. Rothberg notes that most plaques in coronary arteries occur in areas that appeared mild on previous examinations. These plaques do not limit blood flow and may even be invisible to the cardiologist and therefore so imprecise that stents cannot be placed with any certainty.
Where clots form to block blood circulation in coronary arteries is where stents may accurately be placed. But most stents are inserted in patients with stable angina. Stents only prevent symptoms at best and do not prevent heart attacks at their worst. Given the cause of the problem is not addressed, this should not be surprising.
Dr. Rothberg points to 12 studies conducted between 1987 and 2007 involving 5000+ patients and found no reduction in heart attacks attributable to placement of stents. He estimates ~half of cardiac stents are needless.
Dr. Rothberg goes on to say that following a heart attack, arteries remodel (change shape) which is accompanied by an outward rather than inward enlargement. The plaque is hidden from view during a dye imaging test (angiography).
Furthermore, epidemiological evidence shows lower rates of heart disease among populations that consume the most fat. Dr. Rothberg pleads with modern medicine to halt its flawed cholesterol and plumbing analogy in heart disease.
More evidence ignored
Dr. John Mandrola, a non-interventional cardiologist and electro-physiologist, cites two studies in the 1990s which showed the old balloon angioplasty (advancing a wire into a blocked coronary artery and inflating a balloon to break up a clot) relieved angina chest pain but failed to reduce the risk for death.
Dr. Mandrola says bare metal stents made these procedures safer but also did not reduce risk for a heart attack or death.
Dr. Mandrola says a stent may reduce blockage in a coronary artery from 90% to 0% which relieves chest pain, but this effect wanes after just 3 years.
Comparing arterial treatments
In a landmark trial, treatments for patients with multiple impaired coronary arteries and documented oxygen deprivation to the heart (ischemia) were compared. Here are the 10-year survival rates:
Coronary artery bypass surgery 25.1%
Stenting 24.9%
Optimal medical therapy 31.0%
Freedom from angina chest pain 10 years following surgery was as follows:
Coronary artery bypass surgery 64%
Stenting 59%
Optimal medical therapy 43%
This suggests there is a lot of room for improvement
Also recognize, the vast majority of sudden-death mortal heart attacks are electrical storms which are not addressed by coronary artery care. To prevent this type of heart attack, electrolyte minerals would be appropriate, such as magnesium and potassium.
Stent complications
A major drawback of coronary artery stenting is that stents may serve to induce blood clots themselves. Various drugs are slowly released from drug-eluting stents to prevent the overgrowth of reparative tissue that can also block a stent, but the drugs don’t prevent the blood clotting problem. Given that one type of heart attack is defined as a blood clot blocking blood flow in a coronary artery, cardiac stents may represent disease substation rather than disease treatment
A narrowing of the inner diameter of a coronary artery (called re-stenosis) after angioplasty (inflation of a balloon within the artery) ranges from 32-55% and requires re-treatment in 17-41% of patients with bare metal stents.
Drug-eluting stents drop the rate of re-stenosis to less than 10%. These drug-eluting stents have been called “miracle stents.” Miracles they may be, however, over the long term, there is a 40% restenosis rate in stents after 5 years (in diabetics). Major adverse events (heart attacks, within-stent blood clots) after 10 years is ~33%. Despite all the hype, drug-eluting stents have not been shown to reduce all-cause mortality over bare-metal stents.
However, the drugs used within drug-eluting stents may cause what is called stent-edge remodeling and delayed healing that predisposes patients to in-stent closure, sudden blood clots and sudden death. In this instance, the stent has become a problem rather than a solution.
They way out: a red wine molecule
In one experimental animal study, the red wine molecule resveratrol inhibited the re-closure of a coronary artery after stenting or balloon re-opening by 84%.
In another published study the combination use of resveratrol and quercetin, two natural molecules found in small amounts in red wine grapes, work synergistically to inhibit re-closure (re-stenosis) of coronary arteries and are posed as a way for patients undergoing implantation of coronary artery stents to avert complications.
These animal studies carry considerable weight because human studies involving a mortal outcome cannot ethically be conducted. In other words, evaluators can’t wait for human studies to be performed.
Resveratrol has been put to the test in a human trial among patients with stable angina chest pain. Resveratrol (with and without accompanying boron) reduced inflammation (as measure by C-reactive protein – CRP) and improved the quality of life of these angina patients without significant changes in their cholesterol levels. Angina episodes declined by as much as 59% after two months versus 23.8% among patients on standard drug therapy and reduced the need for nitroglycerin tablets. Approximately 80% of patients were satisfied with resveratrol treatment subjectively. Despite this convincing study, resveratrol largely goes unused in cardiology.
Resveratrol as a backstop when all other efforts fail
Factoring for a given failure rate for coronary artery bypass surgery, angioplasty with a balloon to break up clots in coronary arteries and stents implanted within coronary arteries, resveratrol prevents damage to heart muscle even if these adverse events occur. Resveratrol does so by a process called cardiac preconditioning. That is, a low dose of resveratrol activates internal enzymatic antioxidants (glutathione, catalase, SOD) to pre-protect heart muscle should it be subjected to a period of oxygen deprivation.
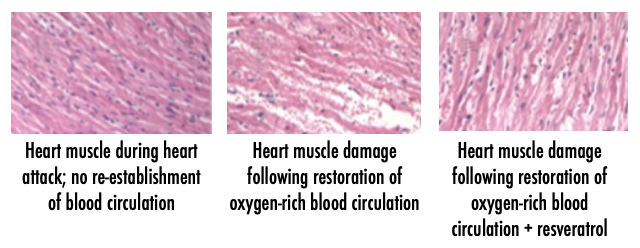
Damage to the heart occurs when circulation is re-established and oxygen-rich blood generates free radicals that damage and permanently scar heart muscle, a problem called reperfusion injury.
It is after a heart attack (blockage of oxygenated blood to heart muscle) when circulation is re-established that oxygen-generated free radicals damage and permanently scar heart muscle, a problem called reperfusion injury. The prior use of resveratrol reduces the size of a heart attack (area of damaged tissue) and minimizes reduction in cardiac pumping.
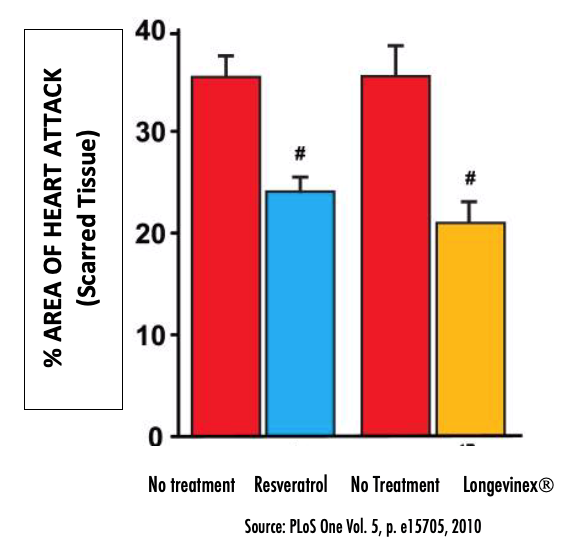
In the animal lab, the use of low-dose resveratrol improves heart function after re-establishment of circulation to the heart. Pre-treatment of resveratrol to animal hearts protects animal hearts from reperfusion injury induced by restoration of oxygenated blood to the heart (see images below).
The only commercially available branded resveratrol to demonstrate this protection in laboratory animals is LongevinexÒ. Formulated as a synergistic combination of resveratrol + quercetin + rice bran IP6, Following an experimentally induced heart attack in the animal lab, LongevinexÒ exhibited superior ability over plain resveratrol to limit damage to heart muscle. Millions more heart muscle cells were spared damage and scarring with LongevinexÒ compared to plain resveratrol.