By Dr. Mercola
According to the Centers for Disease Control and Prevention (CDC),1 approximately 610,000 people die of heart disease in the United States every year. Nearly 735,000 Americans have a heart attack each year. Of these, 525,000 are a first heart attack and 210,000 are repeat heart attacks. Knowing the risk factors, symptoms and taking early action increases the chances of survival.
There are a number of risk factors associated with heart attack. Data published in the Journal of the American College of Cardiology2demonstrates that by following six lifestyle guidelines, women may lower their risk of heart disease by 92 percent and of heart attack by 70 percent. These include eating a healthy diet, getting 2.5 hours of exercise each week, not smoking and limiting alcohol, maintaining a normal weight and watching television no more than seven hours per week.
Stress,3 less than optimal mineral levels,4 daylight saving time5 and even severe emotional loss6 can increase your risk of heart attack as well. While many use the terms “heart attack” and “cardiac arrest” interchangeably, the two conditions are actually different, and knowing the difference can be a matter of life and death.
Heart Attack or Cardiac Arrest?
Sudden, unexpected cardiac arrest is the third leading cause of death in the U.S.,7 which is different from a heart attack. Understanding this difference can help save a life. The most immediately recognizable difference between the two conditions is that a heart attack victim will remain conscious with their heart beating, while someone who suffers from sudden cardiac arrest will be unconscious, with no discernible heartbeat.
Your heart is an extraordinary organ, even continuing to function when it’s detached from your body.8 Since your heart has its own electrical system, as long as it receives an adequate supply of oxygen, it can continue beating. Your heart beats nearly 100,000 times each day and pumps nearly 1 million barrels of blood in an average lifetime. This is enough blood to fill more than three supertankers.
While a heart attack affects the oxygen supply to your heart, cardiac arrest affects its electrical impulses. During a heart attack, part of the heart may have a reduction in oxygen when blood supply is restricted, but the remainder of the muscle continues to beat. During cardiac arrest, the electrical system is negatively impacted by conditions such as cardiomyopathy, heart failure, arrhythmias or ventricular fibrillation.
While heart attacks occur from a lack of oxygen supply and cardiac arrest happens from a disturbance in the electrical system, a heart attack does increase your risk of having a cardiac arrest, and is perhaps the most common reason for this occurrence.9 In other words, loss of oxygen supply to the heart muscle affects the electrical impulses and may trigger cardiac arrest.
As the underlying causative factors of both conditions are different, so too are the symptoms. A heart attack, also called a myocardial infarction, causes injury to the heart muscle. While the heart may continue to beat, the longer you go without treatment the more of the muscle becomes injured and dies. Symptoms of a heart attack can include:10,11
Women sometimes experience additional symptoms, including stomach or abdominal pain, vomiting and weakness or overwhelming fatigue.12 To maximize the odds of survival and minimize permanent damage, it’s important someone experiencing a heart attack receive immediate emergency medical care.
In contrast, electrical problems resulting in cardiac arrest will produce a loss of blood being pumped throughout the body and the brain. Subsequently, the person will suddenly pass out, lose consciousness and their heart will stop beating. In some instances, you may notice some abnormal gasping lasting for a minute or two and in other instances there may be seizure activity at the beginning of the event.13
Emergency Care for Each Condition Is Different
Anyone can provide lifesaving care. Whether an individual suffers a heart attack or cardiac arrest, it’s crucial to immediately call emergency medical services (EMS). Call your local emergency number (911 in the U.S.) and follow the dispatcher’s instructions while waiting for EMS to arrive.
In the case of a heart attack, with each passing minute more of the heart muscle deteriorates and dies,14 so it’s critical to restore blood flow. EMS would rather be called and discover it is not a heart attack than to not be called and the individual die.
If the individual is awake and conscious, ask him or her to lie down and rest until EMS arrives. In many instances a person having a heart attack will deny the severity of their symptoms and insist they’re OK. It is not necessary to have their permission to call EMS, but it is important not to agitate them by insisting they sit down or rest as this only increases the stress on the heart. Instead, you might distract them until EMS arrives by engaging in conversation or asking questions about something other than their health.
In contrast, when an individual suffers a cardiac arrest, the heart immediately stops beating. This means there is no blood being pumped to the body or brain. At this time it is critical for bystanders to call EMS, give CPR (cardiopulmonary resuscitation) and use the nearest automated external defibrillator (AED).
While you may hesitate, being afraid you could hurt the victim, at this time the person is clinically dead and can’t get any worse. Bystander CPR and AED can only help. Additionally, good Samaritan laws provide protection for those who render aid to victims in good faith.15
Sudden cardiac arrest annually affects nearly 326,000 people, approximately 10 percent of whom survive. This number increases to nearly 40 percent when bystanders immediately call 911, start CPR and use AEDs before EMS arrives.16,17 If you don’t have formal training, 911 dispatchers can give you specific instructions on using an AED and performing CPR until EMS arrives.
Bystander Defibrillator Saves Lives
According to the National Heart, Lung and Blood Institute,18 95 percent of people who have sudden cardiac arrest will die from it, whereas rapid treatment with an AED can be life-saving. These machines are lightweight and battery operated. Sticky pads with sensors are attached to the chest and those electrodes send information to the computer inside the machine.
The AED computer will analyze the heart rhythm to determine if electric shock is needed. If required, the machine uses voice prompts to tell you what to do and when to do it. AED machines are safe to use and there are no reports of them harming bystanders or users, or delivering inappropriate shocks.19
In a study by the National Institutes of Health,20 a team analyzed data collected between 2011 and 2015 from six U.S. and three Canadian hospital regions. Nearly 50,000 cardiac arrests occurred outside of a hospital during this period. The team’s analysis demonstrated a greater likelihood of survival when a bystander used an AED rather than waiting for EMS to shock the heart.
The difference was nearly 20 percent greater potential for recovery in those who had early treatment using an AED by a bystander. Additionally, people who were shocked by a bystander had minimal disability after the cardiac arrest versus those whose treatment was initiated by EMS. The more time elapsed, the larger the benefit of bystander AED.21
In a previous analysis of data between 2005 and 2009, the team found approximately 500 more lives could be saved each year in the U.S. and Canada if bystanders used AEDs. Following this and other research, AEDs became more widely available and the team now estimates nearly 3,500 people having a cardiac arrest could be saved by bystander AED use.
Specific Proactive Screenings May Identify Health Problems
By the time you experience symptoms of many diseases, the condition may have already claimed 80 percent of your health. For instance, in the case of heart disease, your first symptom may be a heart attack, and it may claim your life. This means it is critical you proactively use reasonable screening methods to determine your risk of a heart attack, and take preventive measure to avoid a growing disease. Many of the risk factors are modifiable through lifestyle changes. Here are some of the most common risk factors for and indicators of heart attack and cardiac arrest risk:
• Hypertension
In a study at Wake Forest Baptist Medical Center,22 data indicated hypertension was a strong predictor of sudden cardiac death compared to coronary artery disease, which leads to heart attack.
• Body mass index
In the same study, extreme low or high body mass index was predictive of sudden cardiac death, but not coronary artery disease.
• Serum ferritin and GGT
While iron, measured as serum ferritin, is necessary for biological function, excess iron can lead to chronic and deadly conditions such as cancer, heart disease, diabetes and neurodegenerative diseases. GGT is a liver enzyme used in glutathione metabolism and may be used as a screening marker for excess free iron.
The presence of excess stored iron measured by serum ferritin, and free iron measured by GGT are vital indicators to your risk of sudden cardiac death. Maintaining “normal” lab value ranges is not enough to reduce your risk as you’ll discover in my previous article, “Serum Ferritin and GGT — Two Potent Health Indicators You Need to Know.”
• Cholesterol ratios
Your body makes nearly 80 percent of your cholesterol; the rest you get from your diet. If you eat less, your body will make more. The true indicators in your cholesterol numbers are not the total numbers but the ratios between your high density lipoproteins (HDL) to the total cholesterol number and your HDL to triglyceride number. You can find more information about how to assess your risk using your blood results in my previous article, “Cholesterol Plays Key Role in Cell Signaling.”
• Insulin resistance
Many heart attacks are the result of insulin resistance. The higher your insulin resistance, the worse markers such as fasting insulin, triglyceride-to-HDL ratio and HbA1c will be, suggesting you’re at increased risk for diseases such as diabetes and heart disease.
Recent research has demonstrated two specific metrics: Circulating adiponectin and macrophages can with near 100 percent accuracy predict your obese phenotype, meaning whether you’re obese insulin sensitive or obese insulin resistant. By making lifestyle changes I discuss in my previous article, “Insulin, Not Cholesterol, Is the True Culprit in Heart Disease,” you may effectively reduce your risk of heart attack.
An Ounce of Prevention May Reduce Your Risk of Death
Since the first symptom of a heart attack is often a heart attack, there are several strategies you can implement to help prevent heart disease and reduce your risk of death.
Donate blood
If your iron level is high, you’ll want to take steps to lower it. One of the easiest ways to do that is to donate blood on a consistent basis. Interestingly, a study published in the American Journal of Public Health23 found statin cholesterol-lowering medications worked by partially countering the proinflammatory effects of excess iron stores. You can achieve the same effect without the side effects of statin medications by donating blood.
Prepare for daylight saving time
Daylight saving time has been associated with a number of negative health effects, including heart attacks and increased rates of suicide and automobile accidents. You can protect yourself in the spring by following natural strategies to help your body resync after the time change. By waking up 30 minutes earlier on Saturday and Sunday, you’ll minimize the impact of getting up earlier on Monday morning.
Get sunlight early in the morning in order to reduce your levels of melatonin quickly, which will help you get to sleep earlier in the evening. Set your clock ahead on Friday evening so you can adjust more slowly over the weekend.
By optimizing your vitamin D levels and managing your stress you’ll also have less problems falling to sleep. You’ll find specific strategies to help you sleep through the night in my previous article, “Want a Good Night’s Sleep? Then Never Do These Things Before Bed.”
Cyclical ketogenic diet
Lowering your levels of inflammation may also help to lower your risk of heart disease and heart attack. A study from Brigham and Women’s Hospital24 analyzed accumulated data from over 25 years and determined a reduction in inflammation could reduce the risk of a recurrent heart attack. By normalizing your weight and improving your insulin resistance, you’ll also reduce inflammation in your body.
Some of the more significant factors affecting the inflammatory process include an excess of insulin, unbalanced fatty acids, leaky gut, high iron stores and inadequate levels of magnesium. The first three of these can be addressed by choosing a cyclical ketogenic diet as described in my previous article, “A Beginner’s Guide to the Ketogenic Diet: An Effective Way of Optimizing Your Health.”
Magnesium
Magnesium deficiency can trigger a number of health conditions, including anxiety, diabetes, migraines, heart disease and hypertension. Each of these has a significant effect on your cardiovascular health. You can optimize your magnesium levels by eating dark green leafy vegetables or juicing your greens. Other foods rich in magnesium include avocados, seeds and nuts, herbs and spices and fruits and berries. Discover more of how magnesium affects your health in my previous article, “Magnesium An Essential Mineral for Heart Health.”
Monitor cholesterol
For interesting facts about cholesterol and the ratios important to your health, see the following infographic:
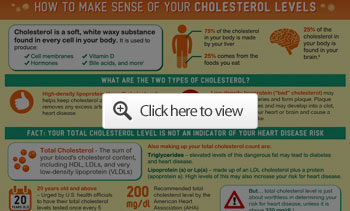
Improve blood flow
There are many factors that can negatively affect blood flow in your body, including a high sugar diet, smoking, electromagnetic forces, stress and high uric acid levels. While repeated blood donations increase the ability of your blood to flow more easily, other strategies you can use include getting enough sensible sun exposure, as this increases the production of a natural vasodilator, nitric oxide.
Earthing or grounding can also help improve a separation of electrical charges and allow your blood to flow against gravity, toward your heart, more easily. The same effect can be achieved by touching another living being, which may be the reason why hugs and pets are so healthy.
Stress
It is important to release the grip stress has over your life as it is a strong predictor of heart attack and stroke. Discover the physical effect stress has on your amygdala, the symptoms you may experience, and successful strategies to reduce stress in your life in my previous article, “How Stress Influences Your Heart Attack and Stroke Risk.”
Sources and References
- 1 Centers for Disease Control and Prevention, Heart Disease Facts
- 2 Journal of the American College of Cardiology, 2015; 65(1)
- 3 Lancet, 2017;389(10071):834
- 4 American Journal of Clinical Nutrition, 2011; 93(2):253
- 5 Reuters, December 16, 2012
- 6 Circulation, 2012; 125(3):491
- 7, 10, 13, 16 Huffington Post, October 25, 2015
- 8 Fact Retriever, November 28, 2016
- 9 American Heart Association, Heart Attack or Sudden Cardiac Arrest: How Are They Different?
- 11 The Hearty Soul, The Surprising Difference Between Heart Attack and Cardiac Arrest
- 12 American Heart Association, Heart Attack Symptoms in Women
- 14 Mayo Clinic, Heart Attack
- 15 US Legal, Good Samaritan Laws and Legal Definition
- 17 Journal of the American College of Cardiology, 2010;55(16):1713
- 18, 19 National Heart, Lung and Blood Institute, Automated External Defibrillator
- 20, 21 National Institutes of Health, March 6, 2018
- 22 Wake Forest Baptist Medical Center, Predictors of Dying Suddenly versus Surviving Heart Attack Identified
- 23 American Journal of Public Health, 2013; 103(4):e105
- 24 Health Canal, 2017; Inflammatory Hypothesis Confirmed: Reducing Inflammation Without Lowering Cholesterol Cuts Risk of Cardiovascular Events





